Hiatus Hernia Repair
What is a Hernia?
A hernia is the protrusion of part of an organ through an opening in the abdominal wall or an opening within the abdominal cavity. It can either be developed at birth (congenital) or it may appear later in life (acquired).
There are natural openings in the wall of the abdomen or within the abdominal cavity that allows certain structures to pass through.
In an acquired hernia, connective tissue degenerates through the process of aging which allows either existing natural openings to widen or new defects to develop in the abdominal wall. This is further mediated by the increase in pressure inside the abdomen leading to a bulge or protrusion of an internal organ out of the abdomen. Some of the factors that contribute to the development of a hernia through the chronic increase in pressure are persistent coughing, obesity, constipation, and frequent heavy lifting. Herniae are also more common in pregnancy, smokers, previous abdominal surgery, and in certain connective tissue disorders.
What is Hiatal Hernia?
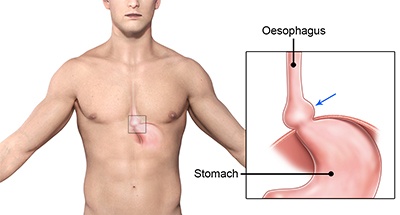
The diaphragm is a sheet of tendon and muscle that separates the abdomen from the throrax (chest). One of the natural openings in the diaphragm is called the Hiatus through which the oesophagus (or gullet) passes through from the thorax to the abdomen in order to join the stomach. In a Hiatus Hernia, the hiatal opening in the diaphragm is widened allowing part of the stomach to protrude into the chest cavity. Hiatus hernia is a common condition that occurs in advancing age and it is highly associated with the development of acid reflux disease (heartburn).
There are four types of hiatus hernia:
Sliding Hiatus Hernia (Type 1): The top portion of the stomach and lower part of the oesophagus (gullet) slide up together through the hiatal opening (or defect) in the diaphragm.
Rolling Hiatus Hernia (Type 2): The junction between the oesophagus and stomach stays in its normal position (below the diaphragm), but part of the stomach roll up into the chest cavity.
Mixed Sliding and Rolling Hiatus Hernia (Type 3): The junction between the oesophagus and stomach slides into the chest cavity whilst part of the stomach has also rolled up into the chest cavity.
Type 4 Hiatus Hernia: The stomach slides into the chest cavity in conjunction with another organ (such as colon, omentum, spleen, pancreas, and small bowel)
Symptoms
A hiatal hernia may not cause any symptoms, but certain individuals may experience heartburn, belching, hiccups, difficulty in swallowing solids or liquids, regurgitation after eating or drinking, and shortness of breath.
Diagnosis
The assessment of a hiatus hernia involves in a combination of a number of investigations such as:
- Barium swallow/meal- A series of X-ray of the oesophagus and stomach are taken during the ingestion of barium liquid and barium-soaked bread to assess the size and type of hiatus hernia. It can also detect any abnormal transit of solids and liquids from the oesophagus to the stomach.
- Gastroscopy- A camera tube is inserted though the mouth into the oesophagus, stomach and first part of the small bowel. The size and type of hiatus hernia and any other associated conditions (such as acid reflux/ reflux oesophagitis) can be diagnosed
- CT scan of chest and abdomen- A 3D mapping of the anatomy may be required for surgical planning in certain instances (ie. where there may be a complex hernia)
Treatment
Management of this condition will need to take into account of the presence and nature of the symptoms as described above. Surgery is usually recommended in patients with acid reflux and obstructive symptoms.
Surgical Procedure
The operation is performed laparoscopically (key-hole surgery) with the patient under general anaesthesia. The surgeon makes 5 small incisions in the abdominal wall through which a camera and surgical instruments can be inserted into.
The first stage of the procedure is the repair of the hiatus hernia which is often associated with reflux disease. Part of the stomach that has moved up into the chest cavity will be pulled back down into the abdomen. The upper stomach and lower oesophagus is dissected away from the surrounding tissue so that they are freely mobilised down into the abdomen without tension.
The hole in the diaphragm (called the hiatus) through which the oesophagus passes is widened in a hiatus hernia. This is partially closed or tightened with sutures so that the hole only permits the oesophagus through. Rarely, an absorbable mesh may be placed around this repair in a very large hiatus hernia or re-do operation which may reduce the risk of recurrence.
The upper part of the stomach (called the fundus) is then partially wrapped and secured around the lower oesophagus with sutures. This manoeuvre is called fundoplication which serves to re-create the valve effect that contributes to the anti-reflux mechanisms.
Risks /Complications of Procedure
Specific side-effect and complications for this operation include:
- Internal bleeding (due to injury to vessels or spleen)
- Infection (including pneumonia)
- Injury to stomach or oesophagus causing perforation
- Swallowing difficulties (due to stomach wrap being too tight)
- Gas-Bloat syndrome (a variable side-effect as a consequence of the stomach wrap)
