Colonoscopy
What is a Colonoscopy?
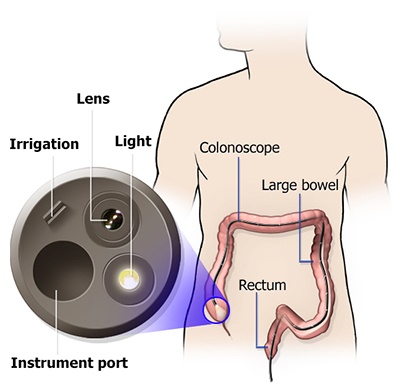
Colonoscopy is an endoscopic procedure performed to allow the specialist to inspect the inner lining of the large intestine (colon and rectum).
The colonoscope is a long, thin, flexible tube with a small video camera and light on the end. Once the colonoscope is inserted through the anus, the surgeon endoscopist can safely guide the instrument through the lower gastrointestinal tract under direct vision to carefully examine the rectum, colon and the last part of the small intestine. The procedure can detect diverticular disease, inflamed colonic tissue, ulcers, abnormal polyp growths, and colorectal cancer. In some cases, therapeutic treatments may be performed at the same time such as the removal of polyp growths and application of rubber bands to internal haemorrhoids.
Indications for Colonoscopy
It may be recommended that you should undergo a colonoscopy if you have any of the following:
- Positive Faecal Occult Blood Test
- Anaemia (Low red blood cell count)
- Iron deficiency
- Rectal bleeding
- Altered bowel habit
- Unexplained weight loss
- Unexplained abdominal pain
- Palpable abdominal mass
- Inflammatory bowel disease (including family history of IBD)
- Abnormal imaging findings of the lower gastrointestinal tract
- Family history of colorectal cancer or cancer-related syndromes
Preparing for Colonoscopy
Your will be provided instructions to help you prepare for the colonoscopy procedure (read downloadable file below). The process is called bowel preparation.
Your large intestine should be devoid of faecal material with only clear or slightly murky fluid remaining. If your bowel is not free of all stools before the procedure, polyps and cancerous lesions can be missed. The colonoscopy may also take longer with increasing risk of complications as the camera views may be partially obscured by faeces. If the bowel preparation quality is poor, then the procedure may need to be repeated or rescheduled.
To ensure good bowel preparation, a strict diet should be followed before the procedure as follows:
For a few days before the colonoscopy, you should start eating a low-fibre (low residue) diet which includes no wholegrains, nuts, seeds, dried fruit, or raw fruits or vegetables. Fruit juices, white bread, refined breakfast cereals, meat and dairy foods are allowed. You should not be drinking alcohol or beverages containing red or purple dye.
On the day before the colonoscopy procedure, you should ideally not eat any solid food. Instead, you can only consume clear liquids like clear broth or bouillon, black coffee or tea, clear juice, sports drinks, popsicles, strained soups, plain jelly, clear fruit cordial (no red/purple colourings), etc.
On the day of the colonoscopy, you remain on clear liquid diet only. You should drink plenty of liquids to stay hydrated, even if you don’t feel especially thirsty.
* Do not eat or drink anything for two hours before the procedure.
A strong laxative will need to be taken and will generally start on the afternoon or evening before the day of colonoscopy (typically 12-18 hours prior) which will loosen the stools and increase bowel movements. Laxatives are usually swallowed as a powder dissolved in water but rarely tablets might be needed.
The bowel preparations (laxatives) you will be prescribed are:
- ColonLYTELY - an oral solution
But alternative preparations may be used such as:
Iron medications produce dark black stools and this makes the view inside the bowel appear dark and there may be an increased risk to the procedure in this setting due to reduced visibility. You should therefore stop taking iron tablets for 5 days before your colonoscopy.
Detailed Instructions for Bowel Preparation
At least 1 week before your procedure, please download and read the file below for instructions on how to prepare for your colonoscopy.
Recovery after Colonoscopy
After the procedure, you may experience a sensation of bloating from the carbon dioxide insufflation of your colon during the procedure. This feeling is of short duration as the carbon dioxide is either absorbed into your body or passed out as flatus. It is not uncommon to pass a small quantity of blood with the first bowel movement after the procedure. You will still require someone to drive you home due to the sedating effects of the medication you have received. A normal diet with increased fluid intake is usually recommended. Consult your doctor if you experience abdominal pain, high fever or increased blood in the stools.
Risks and Complications Associated with Colonoscopy
Colonoscopy is usually a safe procedure but as with any procedure, certain complications can occur. These include:
- Bleeding after a biopsy or polyp removal
- Perforation in the intestinal wall
- Aspiration (with resulting pneumonia)
