Gastroscopy (OGD)
Alt Names: Oesophago-gastro-duodenoscopy (OGD), Upper GI endoscopy
Gastroscopy is a procedure performed using the endoscope to diagnose and, in some cases, provide therapeutic treatments to problems of the upper digestive system.
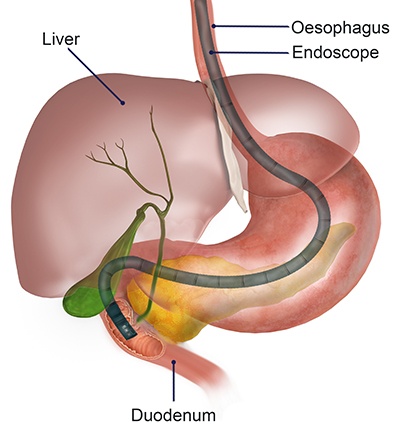
The endoscope is a long, thin, flexible tube with a small video camera and light on the end. Once the endoscope is inserted through the mouth, the surgeon endoscopist can safely guide the instrument through the upper digestive tract under direct vision to carefully examine the inside lining of the oesophagus (gullet), stomach, and the first 2 portions of the duodenum.
Indications for Diagnostic Endoscopy
It may be recommended that you should undergo a gastroscopy if you have any of the following:
- Difficulty in Swallowing
- Vomiting of blood or altered blood (dark)
- Malaena (altered blood in the stools which appears black and runny)
- Anaemia (Low red blood cell count)
- Iron deficiency
- Unexplained weight loss
- Upper abdominal pain/bloating/fullness
- Persistent isolated nausea or vomiting
- Abnormal imaging findings of the upper digestive tract
- Reflux disease/heartburn
- Inflammatory bowel disease
- Coeliac disease
- Liver Cirrhosis
Preparing for Gastroscopy
You should stop eating solid food for 6 hours prior and stop drinking clear fluids for 2 hour before your procedure.
Risks and Complications Associated with Gastroscopy
Gastroscopy is usually a safe procedure but as with any procedure, certain complications can occur. These include:
- Bleeding after a biopsy or polyp removal
- Perforation
- Aspiration (with resulting pneumonia)
